This editorial is based on “Reinforcing the case for a One Health approach” which was published in The Hindu on 07/04/2026. This editorial provides a multidimensional analysis of the One Health approach as a strategic necessity for India’s bio-security. It explores current institutional strides, the socio-economic impact of zoonoses, and practical measures to bridge the gap between environmental integrity and public health governance.
The Covid-19 pandemic exposed that nearly 60% of emerging infectious diseases are zoonotic, underscoring the deep interlinkages between human, animal, and environmental health. Against this backdrop, the One Health approach has gained global traction, reflected in the 2025 WHO Pandemic Agreement and India’s National One Health Mission. With climate change, antimicrobial resistance, and habitat disruption intensifying disease risks, isolated sectoral responses are increasingly inadequate. Thus, One Health emerges as a data-driven, collaborative framework essential for future pandemic preparedness and sustainable public health governance.
What is One Health Approach?
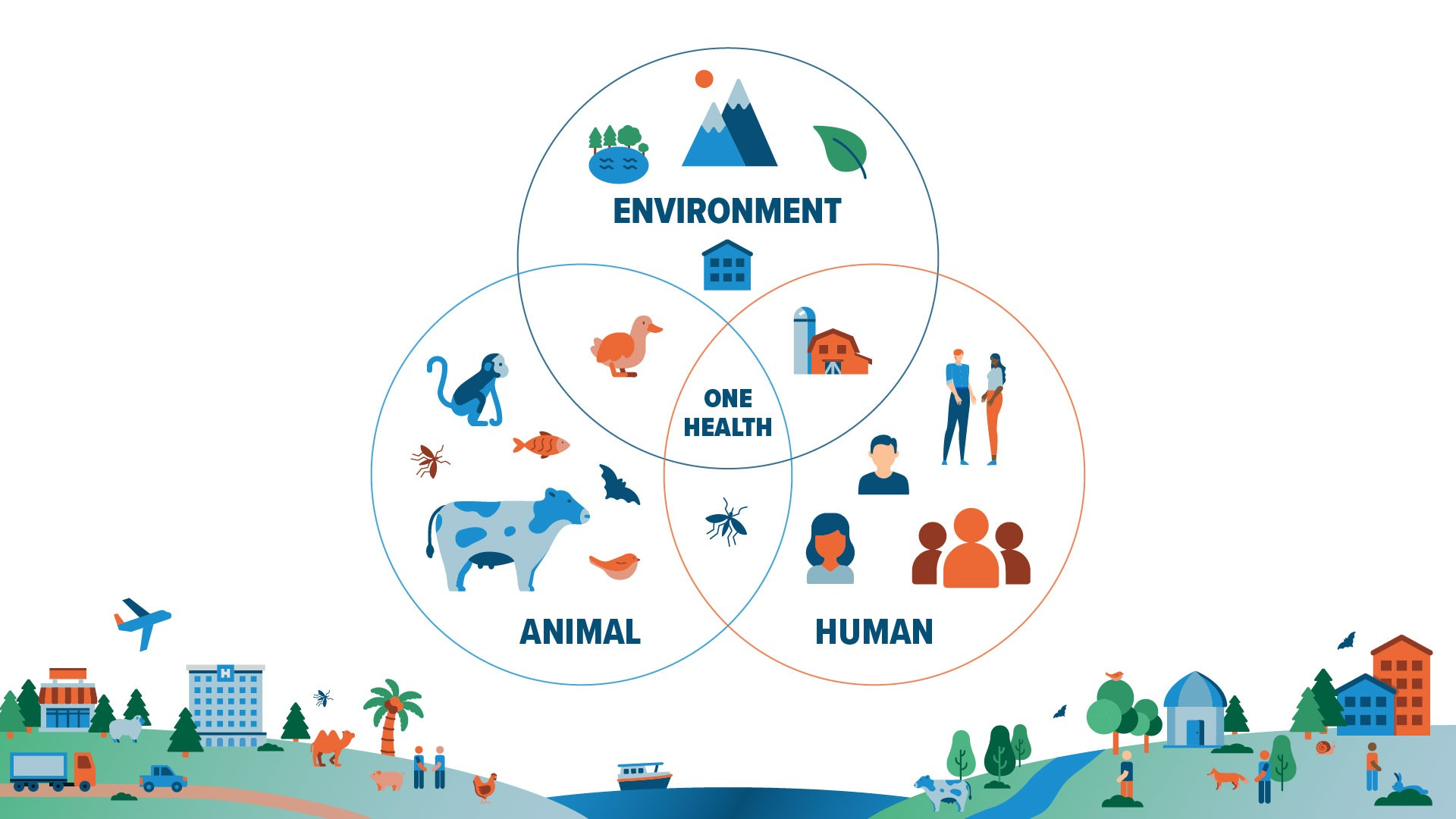
- About : The One Health approach is an integrated, unifying framework that aims to sustainably balance and optimize the health of people, animals, and ecosystems.
- The Three Pillars of One Health: The approach rests on the core idea that we cannot protect one of these areas without protecting the others:
- Human Health: Ensuring the physical well-being of populations and preventing the spread of diseases.
- Animal Health: Protecting wildlife, livestock, and domestic pets from disease and ensuring sustainable agricultural practices.
- Environmental Health: Maintaining healthy ecosystems, clean water, and a stable climate, which are foundational for both human and animal survival.
What is the Need for India to Shift Towards One Health Approach?
- Mitigation of Zoonotic Spillover Risks: India’s high human-wildlife interface makes it a primary theater for “pathogen spillover,” where viruses jump from animals to humans due to habitat encroachment.
- While nearly 60-75% of emerging infectious diseases are zoonotic, India currently monitors these in silos, often missing early warning signals in wildlife.
- The International Livestock Research Institute reports that 13 zoonoses are responsible for 2.4 billion human disease cases and 2.2 million deaths in India annually.
- Combating the “Silent Pandemic” of AMR: Antimicrobial Resistance (AMR) in India is fueled by the interconnected use of antibiotics in human medicine, poultry, and aquaculture, leading to “superbugs” in the environment.
- Without a One Health lens, regulating antibiotic runoff from pharmaceutical hubs or livestock feed remains impossible, rendering life-saving drugs ineffective.
- India’s NAP-AMR 2.0 (2025–2029) highlights that multidrug resistant pathogens contribute significantly to hospital mortality, studies show antibiotic-resistant bacteria are now prevalent in effluent samples from major Indian river systems.
- Securing the World’s Largest Livestock Economy: Livestock Sector is an important subsector of agriculture in the Indian economy. It grew at a Compound Annual Growth Rate (CAGR) of 12.77% from 2014-15 to 2023-24, yet it remains vulnerable to transboundary diseases that devastate rural incomes.
- A One Health approach integrates veterinary surveillance with public health, ensuring that diseases like Foot and Mouth Disease (FMD) or Lumpy Skin Disease do not cripple the agrarian economy.
- The 2025 livestock census confirms India manages over 535 million animals, yet the poultry industry alone has faced massive loss due to Avian Influenza.
- Climate-Induced Disease Pathshift: Climate change is altering the geographical range of vectors like mosquitoes and ticks, pushing “forest diseases” into urban centers and vice versa.
- Rising temperatures and unseasonal floods accelerate the maturation of pathogens, requiring an integrated climate-health surveillance system to predict new outbreak clusters.
- The State of India’s Environment 2026 report reveals that extreme weather days (267 in Himachal, 173 in Kerala) have triggered a surge in vector-borne shifts.
- Consequently, India has seen a rise in Dengue and Malaria cases in previously “low-risk” high-altitude regions.
- Biodiversity Conservation as a Health Shield: Intact ecosystems act as “biological buffers” that dilute pathogen concentration, however, India’s rapid land-use change is destroying these natural firewalls.
- Maintaining biosphere integrity is a public health strategy, as fragmented forests force species like bats and primates into closer, dangerous contact with human settlements.
- Recent studies confirm that land-use change (deforestation, urbanization, and agricultural expansion) is the leading driver of emerging infectious diseases (EIDs).
- Enhancing Pandemic Preparedness & Intelligence: The One Health framework facilitates the transition from “reactive compensation” to “proactive prevention” by leveraging AI and genomic sequencing across sectors.
- By creating a unified data ledger between the ICMR (human) and IVRI (animal), India can detect “Pathogen X” in a forest before it reaches a city hospital.
- The National One Health Mission (2026) is establishing BSL-3/4 labs, this is critical as actions to prevent disease outbreaks carry estimated returns of up to 86%, delivering both direct savings from avoided healthcare costs and indirect benefits that protect agricultural productivity and food security.
- Food Safety and Nutritional Security: Contaminated food chains, often due to pesticides or zoonotic pathogens in meat, directly impact India’s “National Nutrition Mission” (Poshan Abhiyaan).
- Foodborne diseases cost India roughly $15 billion annually in lost productivity, reflecting a significant economic burden.
- They lead to increased healthcare expenditure, reduced workforce efficiency, and long-term impacts on human capital.
- One Health ensures “Farm-to-Fork” safety by monitoring soil health, irrigation water quality, and veterinary drug residues, which are vital for a healthy, productive workforce.
- Foodborne diseases cost India roughly $15 billion annually in lost productivity, reflecting a significant economic burden.
- Strategic Global Leadership (Viksit Bharat @ 2047): For India to lead the Global South, it must pioneer a scalable One Health model that balances development with ecological safety.
- By successfully implementing the National One Health Mission, India sets a template for tropical, high-density nations to achieve the Sustainable Development Goals (SDGs) while protecting their GDP.
- The Union Budget 2026–27’s 24% increase in allocation to the Department of Health Research (over ₹4,821 crore) can act as a critical enabler, strengthening integrated research and surveillance systems and positioning India as a global exemplar in One Health–driven governance.
What Key Strides India has Taken Towards One Health Approach?
- Institutional Governance via National One Health Mission (NOHM): Breaking historical administrative silos, India has aggressively centralized its bio-security governance to seamlessly manage the human-animal-environmental interface.
- The Mission was launched following the recommendation of the 21st Prime Minister’s Science, Technology and Innovation Advisory Council (PM-STIAC) and received Cabinet approval in February 2024.
- It is being steered by the Office of the Principal Scientific Adviser (OPSA) to the Government of India, with participation from over 16 Central Ministries and Departments, including the Ministry of Ayush.
- The Department of Health Research (DHR), along with the Indian Council of Medical Research (ICMR), acts as the implementing agency.
- Anchor Research Infrastructure at National Institute for One Health, Nagpur: To bridge the massive research deficit in cross-species pathogen spillover, India has established a dedicated epicenter for integrated genomic and epidemiological research.
- This centralized anchor institution coordinates nationwide biosurveillance, standardizing protocols to predict and intercept zoonotic threats before they escalate into human epidemics.
- Livestock Defense under Animal Pandemic Preparedness Initiative: Recognizing that agrarian livestock health is inextricably tied to human bio-safety and economic stability, India has strategically overhauled its veterinary defense framework.
- This initiative transcends routine immunization, constructing a systemic “Farm-to-Fork” defense mechanism grounded in active genetic surveillance and robust community capacity building.
- Supported by a ₹1,228.70 crore financial provision and World Bank funding under the Animal Health System Support for One Health project, the APPI is actively deploying across 151 vulnerable districts.
- Combating Antimicrobial Resistance via NAP-AMR 2.0 (2025-2029): Tackling the silent pandemic of drug-resistant pathogens, India is aggressively pivoting to regulate antibiotic runoff across pharmacological, agricultural, and clinical domains.
- By adopting a stringent multi-sectoral regulatory posture, the nation aims to halt the environmental proliferation of “superbugs” that neutralize life-saving medical interventions.
- Decentralized High-Risk Pathogen Surveillance Networks: Addressing dangerous resource asymmetries in diagnostic capabilities, India is rapidly decentralizing its advanced pathogen detection and containment infrastructure.
- This strategic expansion weaves a resilient geographical safety net, empowering localized metagenomic sequencing and rapid syndromic surveillance during localized emerging outbreaks.
- The Integrated Disease Surveillance Programme (IDSP), active since 2004, monitors and responds to over 33 communicable diseases across all 36 States/UTs.
- IDSP employs District Public Health Laboratories (DPHLs) and State Referral Laboratories (SRLs) for disease surveillance and media scanning to enhance early outbreak detection and response.
- Ecological and Climate-Health Convergence Integration: Acknowledging that climate change and rapid biodiversity loss act as dangerous threat multipliers for disease transmission, India is directly intertwining ecological preservation with public health.
- This holistic dimension recognizes intact ecosystems as necessary biological shields, actively mitigating the dangerous “edge effect” where deforestation forces stressed wildlife into human settlements.
- Recent initiatives are actively mapping the climate-induced spatial migration of diseases like Dengue into high-altitude zones, utilizing environmental integrity as a quantifiable metric for health security.
- Grassroots Capacity via Field Epidemiology Program (FEP-OH): Recognizing that early outbreak detection relies entirely on grassroots operational competence, India is systematically overhauling its human resource training to reflect the One Health Triad.
- This educational restructuring ensures that frontline health workers, wildlife wardens, and medical officers utilize a unified tactical framework during complex cross-species outbreak investigations.
- Also, under the PM-ABHIM scheme and ‘Programme for Strengthening Research & Development towards integrated disease control and pandemic preparedness for the National One Health Mission’, there is a provision for community engagement, risk communication, and capacity building including training and workshops of the stakeholders.
What Measures are Required to Effectively Operationalise The One Health Approach in India?
- Decentralized Village-Level Bio-governance: Empowering grassroots institutions like Gram Panchayats and local water sanitation committees is crucial for establishing a localized, real-time epidemiological defense line.
- By training community para-veterinarians and village health workers in syndromic surveillance, early signs of wildlife mortality or waterbody contamination can be intercepted immediately.
- This decentralized administrative structure transforms passive rural communities into proactive sentinels of global bio-security. It inherently builds a resilient, ground-up early warning pipeline that effectively bypasses traditional bureaucratic reporting delays.
- Deeptech and AI-Driven Predictive Metagenomics: Operationalizing advanced artificial intelligence and machine learning pipelines is necessary to cross-analyze disparate datasets encompassing satellite climate anomalies, human clinical symptoms, and livestock morbidity.
- This technological integration shifts the paradigm from retrospective epidemiological tracing to highly predictive, autonomous bio-surveillance algorithms capable of anticipating outbreak hotspots.
- By synthesizing real-time metagenomic sequencing with environmental monitoring sensors, policymakers can instantly detect novel pathogen signatures.
- This establishes an active digital shield that triggers automated containment protocols long before urban transmission occurs.
- Legislative Integration and Statutory Mandates: Moving beyond ad-hoc administrative task forces requires structurally anchoring the One Health framework within robust, constitutionally grounded public policy legislation.
- Enacting strict statutory mandates forces historically siloed ministries of health, agriculture, and environment to seamlessly share classified epidemiological intelligence without jurisdictional friction.
- This formal legal architecture ensures that cross-sectoral collaboration is a compulsory administrative duty rather than a voluntary inter-departmental exercise.
- Consequently, it creates a unified regulatory environment capable of swiftly enforcing sweeping bio-security directives during emerging crises.
- Agroecological Transitions to Natural Farming: Systematically incentivizing the large-scale transition from chemical-intensive agriculture toward sustainable natural farming methodologies is a fundamental preventative health strategy.
- This ecological shift actively restores depleted soil microbiomes, drastically reducing the environmental accumulation of veterinary antibiotic runoff and toxic pesticide residues that fuel antimicrobial resistance.
- By deeply integrating agronomic sustainability with human nutritional security, this measure structurally fortifies the “Farm-to-Fork” continuum.
- It fundamentally severs the dangerous chemical pathways that currently compromise both ecosystem vitality and human immunity.
- Wetland and High-Altitude Ecosystem Preservation: Strategically enforcing the structural conservation of fragile geographical biomes, particularly critical wetlands and sensitive Himalayan ecosystems, acts as a primary biological shield against pathogen spillover.
- Maintaining pristine ecological integrity actively dilutes viral concentrations in wildlife while simultaneously minimizing the dangerous “edge effect” caused by anthropogenic encroachment.
- This proactive environmental management ensures that stressed zoonotic reservoirs remain isolated within their natural habitats rather than interacting with human peripheries.
- It firmly establishes biodiversity conservation as an indispensable, non-negotiable pillar of national health defense.
- Fiscal Consolidation via One Health Budgeting: Re-engineering macroeconomic planning to incorporate dedicated “One Health Budgeting” ensures that proactive pandemic preparedness receives sustained, non-lapsable sovereign funding.
- By structurally linking state fiscal health and debt consolidation strategies with proactive investments in bio-security, governments can transition from reactive disaster financing to preventative economic resilience.
- This financial paradigm mandates that infrastructural allocations actively account for ecological and public health risk assessments prior to approval.
- Ultimately, it aligns long-term economic nationalism directly with the preservation of global health security.
- Climate-Health Synergy in Decarbonization Infrastructure: Integrating epidemiological risk forecasting into the deployment of large-scale climate mitigation technologies, including carbon capture and storage networks, addresses the intersection of industrial transition and bio-safety.
- As national policies actively pursue ambitious carbon reduction targets, it is imperative to ensure these infrastructural shifts do not inadvertently disrupt local ecosystems or displace wildlife vectors.
- This holistic planning rigorously evaluates how localized atmospheric and temperature modifications influence the spatial migration of vector-borne diseases.
- It guarantees that climate engineering actively synergizes with public health stability.
- Digital Regulation for Infodemic Management: Instituting stringent regulatory frameworks across social media ecosystems is critical to algorithmically suppress the rapid proliferation of unscientific health misinformation during cross-species outbreaks.
- By legally requiring digital platforms to prioritize verified epidemiological directives from unified public health authorities, governments can effectively neutralize the panic-driven “infodemics” that undermine containment efforts.
- This active digital governance ensures absolute public compliance with complex biosecurity protocols, ranging from localized culling operations to urgent vaccination drives.
- It transforms digital networks from vectors of panic into tools for coordinated societal resilience.
Conclusion
The One Health approach represents a critical paradigm shift from reactive crisis management to proactive, ecosystem-based bio-security. By integrating human, animal, and environmental health into a single governance framework, India can effectively mitigate zoonotic threats and the burgeoning AMR crisis. Ultimately, operationalizing this multidimensional strategy is not merely a health preference but a foundational requirement for achieving the vision of a resilient and Viksit Bharat by 2047.
|
Drishti Mains Question
The frequent outbreaks of zoonotic diseases in India are a manifestation of ecological imbalance.” In light of this statement, evaluate the significance of the National One Health Mission in strengthening India’s pandemic preparedness
|
FAQs
Q. What is the One Health Triad?
It is the functional intersection of human health, animal health, and environmental/ecosystem health.
Q. Which global bodies lead the One Health initiative?
The Quadripartite Alliance, comprising the WHO, FAO, WOAH, and UNEP.
Q. What is a zoonotic spillover?
The transmission of a pathogen from a vertebrate animal to a human host.
Q. Where is India’s premier One Health institute located?
The National Institute for One Health (NIOH) is located in Nagpur.
Q. How does climate change affect One Health?
It acts as a threat multiplier by altering vector habitats and forcing wildlife-human contact.
UPSC Civil Services Examination, Previous Year Questions (PYQs)
Mains
Q. “Besides being a moral imperative of a Welfare State, primary health structure is a necessary precondition for sustainable development.” Analyse. (2021)