Social connections, physical health, freedom from chronic pain, and spiritual engagement are associated with increased likelihood of complete mental health (CMH) among adults age 65 years and older, according to a new nationally representative study of Canadian seniors.
Other characteristics associated with CMH include male sex, being married, and having no history of depression, anxiety, or substance use disorder.
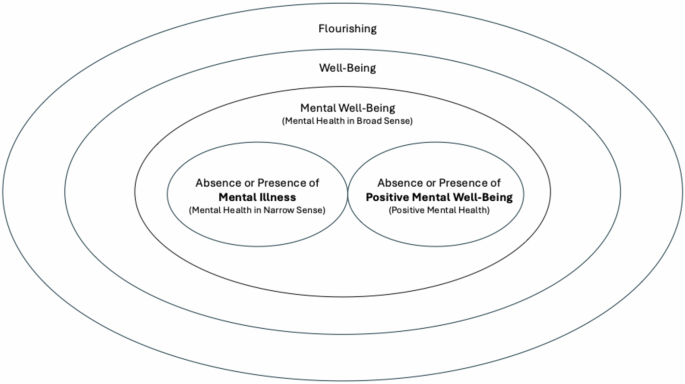
“Over the past few decades, mental health research has primarily focused on mental illnesses, including depression, anxiety disorders, and schizophrenia. However, emerging literature has increasingly emphasized the need to reconceptualize mental health not solely as the absence of psychopathology, but as the presence of positive psychological attributes,” wrote the authors.
The study was published April 8 in PLOS One.
Many Older Canadians Flourishing
“Mental health in later life is not just about avoiding mental illness, it’s about flourishing,” senior author Esme Fuller-Thomson, PhD, director of the Institute for Life Course & Aging and professor in the Factor-Inwentash Faculty of Social Work at the University of Toronto, told Medscape News Canada.

“Strong social connections, good sleep, and being free of chronic pain are key factors that help older adults thrive. The good news is that more than 90% of older adults are free of all mental illnesses, and approximately three-quarters of older adults are experiencing high levels of happiness and social and psychological well-being,” Fuller-Thomson said.
“I spent the first 25 years of my career studying mental illness, but I became increasingly interested in what helps people truly flourish, not just survive. That means feeling happy and satisfied with life, having strong social and psychological well-being, and being free from mental illness. With Canada’s aging population, it’s critical that we focus on the modifiable factors that help older adults thrive,” she said, explaining why she decided to explore this topic now.
Using the 2022 Mental Health and Access to Care Survey, the researchers identified factors associated with the absence of psychiatric disorder (APD), which is defined as the absence of suicidality, bipolar disorder, major depressive episode, anxiety disorder, and substance use disorder in the past year. They also sought the factors associated with CMH — defined as APD, life satisfaction or happiness almost every day in the past month, and social and psychological well-being almost every day in the past month. The survey included a nationally representative sample of 2024 Canadians aged 65 years or older.
Factors associated with ADP and CMH among older adults included male sex, married status, having social support, reporting religious or spiritual beliefs to be important, and having excellent self-reported health.
In addition, respondents without chronic pain, who had no difficulties in instrumental activities of daily living, had no sleep problems, and no history of depression, anxiety, or substance use disorder also had increased odds of both ADP and CMH.
Highlighting a Positive Reality
“Social support stood out. Older adults with strong support had twice the odds of complete mental health. Not surprisingly, good sleep, absence of chronic pain, and better physical health were also strongly associated with flourishing. We hope this encourages a more holistic approach to care that goes beyond treating illness to promoting well-being,” Fuller-Thomson said.
“The good news is that many key factors, like sleep, pain, and social connection are modifiable. Just as importantly, about three-quarters of older adults are flourishing, and we want to highlight that positive reality rather than reinforce the overly negative narratives that too often dominate discussions of aging,” she said.
Family doctors and geriatricians should consider asking their older patients about social isolation, sleep, and pain, Fuller-Thomson suggested. “These are central to mental health and well-being, they are not secondary concerns. Addressing them proactively may make a real difference in whether patients simply survive or truly thrive in optimal mental health,” she said.
Three Pillars of Well-Being
Commenting on the study for Medscape News Canada, Simon B. Sherry, PhD, professor of psychology and neuroscience at Dalhousie University in Halifax, Nova Scotia, said, “This study highlights three pillars of well-being in later life, which are social connection, restorative sleep, and effective pain management. These are meaningful, modifiable targets for clinicians working with older adults.” Sherry did not participate in the research.

“At the same time, however, because the data are cross-sectional, we can’t determine directionality. Strong mental health may just as easily lead to better sleep, less pain, and richer social engagement. For example, individuals struggling with depression or anxiety often withdraw socially, sleep poorly, and experience heightened pain sensitivity,” he said. Longitudinal research is needed to clarify these pathways, Sherry added.
“Still, the study highlights modifiable domains that clinicians already know matter. Social connection, sleep, and pain are all viable targets in psychological treatment and are especially relevant in aging populations, where isolation, insomnia, and chronic pain are common. This work adds to a growing conversation about holistic, upstream approaches to supporting mental health in older Canadians,” he said.
The study was funded by the Public Health Agency of Canada’s Federal Student Work Experience Program. Fuller-Thomson and Sherry reported no relevant financial relationships.